Let’s Talk Science and My Disabling Autoimmune Disease
I’m willing to bet that none of you have heard of, nor know how to pronounce the diagnosis I received about a year ago. I sure didn’t, that’s for sure.
Ankylosing spondylitis. Anka-what? That was my response when I first read about it. But - let’s back up a bit, it’s a good story if you like wild rides.
In approximately late 2019-early 2020, I started noticing that every time I got sick, I started having this weird pain in my jaw, back, and legs that I had never noticed before. It was excruciating and unlike anything I’ve ever felt. Since it was only when I was sick, I didn’t think much of it. However, towards the end of 2020, I started experiencing the pain randomly, and it wasn’t just when I was sick. It was so severe that it would confine me to bed, because I literally couldn’t walk. While it wasn’t super often, the fact that it was starting to happen when I wasn’t sick, had me a little concerned.
The only way I have ever known how to accurately describe what it feels like for someone who has never felt it, is that it feels like someone is breaking my bones in slow motion, for hours upon hours. During a flare, the pain starts in my lower back, and I feel it through my hips, pelvis, knees, and down to my toes. I noticed it was always symmetrical - meaning I felt it on both sides, in both legs, hips, etc.
In 2021 my flares were getting even worse and more frequent. I also met the man who would eventually become my husband. I had told him about these flareups and about the pain. He watched the flareups get worse and more frequent as time went on. Eventually, it got to the point that I was unable to take care of myself if I was experiencing a flareup. He had to help me walk from bed to the bathroom, help me in and out of the shower, I had to shower with a shower chair, I wasn’t able to drive, I had several bad falls because my legs would just completely give out on me - it was the most debilitating thing I had ever physically experienced. I had to start using a cane, and I had even looked at wheelchairs that I could possibly use when I had a flareup so I could perform even just basic tasks. I couldn’t take the pain any longer and I knew I needed to do something.
My primary care physician is an angel on earth, so I went to see her. She ordered routine lab work, but she also included what’s called your CRP and ESR (sed-rate) which are categorized as inflammatory markers, as well as screenings for lupus and rheumatoid arthritis. Lupus and RA were both negative.
My CRP’s and and sed-rate though? Through the roof. These markers are used to measure, detect, and monitor acute or chronic internal inflammation. They are most commonly found in autoimmune diseases, but they can also be elevated in cancer, infections, or cardiovascular issues. Given the fact I didn’t have cancer, an infection, or cardiovascular issues, that told us I was likely dealing with some kind of autoimmune issue, but she couldn’t tell me what. She was, however, very concerned by my inflammatory markers, especially my CRP. For perspective, the lab we used measures your CRPs from 0.0-0.5mg/dL. Anything over 0.5 was considered elevated. Although, depending on the person, sometimes 1.0 levels could be considered normal. Anything over that usually indicates active and significant inflammation. At that time, my CRPs showed I was at 54. To my PCP and me, that was jaw dropping. She prescribed a 10 day steroid and I felt like a million bucks for 10 days. She said this told her that the inflammation was a major problem, and that we needed to find out what was causing it.
She immediately sent me to a rheumatologist. She let me choose which one I wanted to see. I found someone I was hopeful about. I was dead wrong. This man had terrible bedside manner and was extremely brazen and, in my opinion, very rude. I was told that the pain I was experiencing was without a doubt, fibromyalgia. When I asked him what he recommends for treatment, he said he doesn’t treat fibromyalgia with anything other than exercise. I asked him how I was supposed to exercise during a flareup when I couldn’t even walk, and he didn’t have an answer. When I asked how the elevated inflammatory markers are explained, since fibromyalgia doesn’t typically cause them to be elevated, I was told my weight was the reason.
Now, here’s the thing - I wasn’t looking for pain medication. I was looking for an answer that explained why I was feeling the way I was feeling and what he told me just didn’t sit right. I’m a firm believer that you know your body best, and if you know something isn’t right, you should listen to your body. I have seen too many family and friends, and fellow disability advocates know something is wrong but are told it’s nothing serious by doctors, and by the time the doctors realized it was actually something serious, it was too late. I KNEW something wasn’t right and I KNEW that fibro didn’t explain anything for what I was experiencing. I went back to see my PCP, and she agreed. She told me to find a new rheumatologist and that in the meantime, she was going to send me to a neurologist so they could rule out anything neurological. At this point, my flareups were at least 5 times a week, and the pain was getting significantly worse with no explanation as to why. The flareups occurred with both rest and activity, I eliminated gluten and dairy thinking that could be a trigger, and it made no difference. It seemed like no matter what I did, there was no rhyme or reason to the flares and there was nothing I could do to improve them or prevent them.
The neurologist I saw was fantastic and validated the pain I was feeling. She eliminated multiple sclerosis, a rare form of neuropathy, and several other conditions that I can’t even remember at this point. She was so sympathetic, and felt awful that she couldn’t give me any answers, but encouraged me to keep searching and fighting.
So that’s what I did. I somehow managed to get Mayo Clinic to take me as a patient (way, way harder than you think it is if you don’t have a diagnosis), and that was shockingly a joke. I was told it was a combination of fibromyalgia and sleep apnea….. lol
I found a new rheumatologist. They did every kind of imaging you can think of, the amount of blood tests I did was astounding. There were still no answers. They “diagnosed” me with an unspecified autoimmune disease. They said they couldn’t tell me exactly what it was, but that they at least knew it was autoimmune. They prescribed me 2 different immunosuppressants. Both of these actually helped slightly, as my flares decreased to about 3-4 a week and they also lowered my inflammation slightly. My CRPs sat in the 30s for a while, but still way too high. The office I was going to had turned over several doctors, and each of them said the same thing - an unspecified autoimmune disease.
I went in for my routine follow up for refills in January of 2025 and in walks this new doctor - again. She wasn’t new, come to find out. She had been with the office for 7 years, and also assured me she wasn’t going anywhere. This lady LISTENED. She ASKED questions and she was the ONLY rheumatologist to do a physical exam of me. At the end of the exam, she told me that she strongly believed I had ankylosing spondylitis. She said she wanted to run labs for a genetic marker called HLA-B27. 90% of patients with AS have this marker. She did say that some people with AS don’t have the genetic maker so it doesn’t necessarily mean you don’t have AS if you don’t have the genetic marker, but she wanted to know whether or not I did. The genetic test came back negative (which was great news, as I knew I would eventually be starting a family) but at my next follow up, she said that she was certain I had AS, even without the genetic marker.
This conversation occurred in February 2025. This all started 5 years before, that’s how long this journey was for me. They say it takes an average of 6 years for someone to receive an autoimmune diagnosis. This is because there are literally hundreds, it’s so broad, and so many of them mimic each other in symptoms too.
She asked me how I felt about the idea of adding another medication. I told her that if it was another immunosuppressant, that I wasn’t entirely interested, as I felt the 2 I was already on hadn’t made as much of a difference as I was hoping and it didn’t make sense to add yet another one. She said “I was thinking something much stronger.” I was very clear I didn’t want any sort of pain medication that was going to impact how tired I was during the day, as I needed to be able to work. She said she wanted me to try Humira, and that it was not a pain medication, it was a biologic. Most of you have probably seen commercials for it. It’s most commonly prescribed for rheumatoid arthritis, crohn’s disease, psoriatic arthritis, and ankylosing spondylitis. At the end of the commercial, you always hear “if you can’t afford your medication, Abbvie may be able to help.”
She explained that it was a twice a month injection and is a biologic, that targets your TNF inhibitor aka it’s a TNF blocker. A TNF blocker targets your Tumor Necrosis Factor (TNF), a protein that causes inflammation.
To me, this meant we were going to be targeting what started all of this - the internal inflammation I had for years and THAT’S what I had been fighting for the entire time.
Now, this medication is extremely expensive. For a 1 month supply, my insurance is billed over $6,000. My co-pay is $250, and because Abbvie (the manufacturer) needs people to take this medication for research purposes, they pay for my co-pay. I pay absolutely nothing for this magical pen of liquid that has literally changed my life. When I first started it, Abbvie provided a registered nurse at no cost to FaceTime me and walk me through exactly how I should be self-administering it. I was able to ask any and all questions that I had about storing the medication (it has to be refrigerated), that my doctor couldn’t answer. For the first few months, Abbvie provided a patient advocate that would call me periodically to see how I was doing, to see if the Humira was working, and how it may be helping me for their research purposes.
Now? My flareups are down to only once or twice a month AT THE MOST. The best part? I SEE the difference because my inflammatory markers are NORMAL. My CRPs have been sitting at 1.5. I went from the 50s to normal because of this medication. We have eliminated one of the immunosuppressants and will soon eliminate the other.
Now, what is ankylosing spondylitis? I saved the best part (the medical nerd in me) for last.
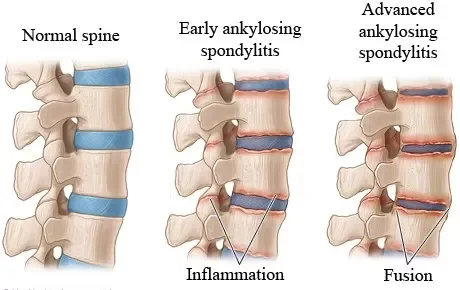
AS is a rare and chronic inflammatory arthritis that primarily affects the spine, sacroiliac joints (the part of your spine that connects to your pelvis), and hips. In some cases, it can also affect the jaw, knees, and ankles. AS can lead to permanent spinal deformity, significant mobility loss, and a higher risk of fractures. Over time, bones can calcify and fuse, limiting movement and posture. Unfortunately, there is no cure, but there are treatments and lifestyle changes that can help. Humira being one of those. Only about 0.2-0.5% of the US population have AS. 54% of those people go undiagnosed for at least a decade. For me, AS is debilitating. It significantly limits my ability to perform major life activities. Before I started the Humira, there were days I couldn’t go to work and I couldn’t function alone during a flareup.
The Humira has been lifechanging for me. I was able to get pregnant and have minimal flareups during that pregnancy. I hardly ever have to call in to work anymore. I haven’t had a fall since I started it. The flareups are few and far between. I can take my dogs for a walk without the fear that I would have a flareup after. I can get up from a sitting position without needing assistance. I can get in and out of the shower without assistance. I can walk to the bathroom without assistance.
I don’t know what it will look like down the road. There’s the fear of spinal fusion and other complications. But for now, I’m soaking up the freedom the Humira has given me for as long as I can. Big pharma loves to suck money out of us, but given the fact that I don’t pay a dime for it, I can honestly say that I am a perfect example of it actually working and they aren’t even getting money out of me directly.
Huge shoutout to my husband for sticking by my side through the worst parts. The flares, the pain, the tears, the humiliating moments I had to ask for help. Chronic pain is a bitch. Sometimes it’s difficult for the people who love us to understand it if they have never experienced it. He has always done his best to be understanding, but I do know it’s hard for him to imagine what it actually feels like. One of his best friends actually has the same diagnosis and is also on Humira. This was cool for me because he had the same symptoms and inability to walk, and he was able to also explain that to my husband. For him, it was cool to hear from someone else what it’s also like. For me, it was cool to know that someone in our life also knows exactly how I feel.
The disabilities I experience that require the use of a service dog are all invisible. This was the first time I had ever experienced a visible disability in my lifelong journey of the American healthcare system. If there is any advice I can give any of you who know something is wrong but can’t get an answer, it’s keep fighting. You know when something isn’t right. If you’re told it’s one thing but you just know in your bones that it’s not that, keep looking, keep searching, keep fighting. Autoimmune diseases are so complicated and there are so many that some rheumatologists don’t even know about and they’re the ones who are supposed to be treating them.
Thanks for coming to my science talk.